What Are Truck Weigh Stations and How Do They Protect You?
According to TRIP, Tennessee’s freight system moved 552 million tons of freight in 2022. In recent years, Tennessee has become an increasingly busy hub for commercial freight vehicles, and we are likely to see even more freight being moved across our state in the years ahead. While commercial trucks play an integral role in our…
Read MoreWhat is the Last Clear Chance Doctrine, and Could It Help Your Case?
In a personal injury case, the most pressing question for the involved parties is usually who to blame. Individuals on all sides of an accident can easily start pointing fingers at one another as they try to sort out who should bear the brunt of responsibility and front the cost of any resulting losses. In…
Read MoreBe Wary of Electric Bikes
Electric bikes have grown rapidly in popularity. In 2026, it is not uncommon to see multiple e-bike riders while on your way to work. These bikes appeal to a wide range of users, from those who use them as their primary form of transportation to those who only use them for quick trips. But regardless…
Read MoreElectric Scooter Laws and Injuries in Nashville
Electric scooters are a common sight in Nashville, particularly in high-traffic downtown areas and neighborhoods that see lots of tourists. While electric scooters do provide a convenient way to get around, they are also fairly risky. Electric scooter accidents leave victims wondering who is responsible for their injuries and if they are entitled to compensation…
Read MoreWhat Are “Damages” in a Car Accident Case in Tennessee?
After a car accident, you may be focused on fault—who caused the accident, what went wrong, and what your insurance company is going to say. But damages are an equally important part of this equation. Once you have figured out who is to blame for the accident, you may be able to recover compensation for…
Read MoreRocky McElhaney Law Firm Continues Streak with 12th “Best Places to Work” Recognition
We’re proud to announce that Rocky McElhaney Law Firm earned recognition in Nashville Business Journal’s 2026 “Best Places to Work” list. This win marks our 12th year and puts us “among the best in Nashville for employee satisfaction and the ability to have fun while finding success.” What this recognition represents The Best Places to…
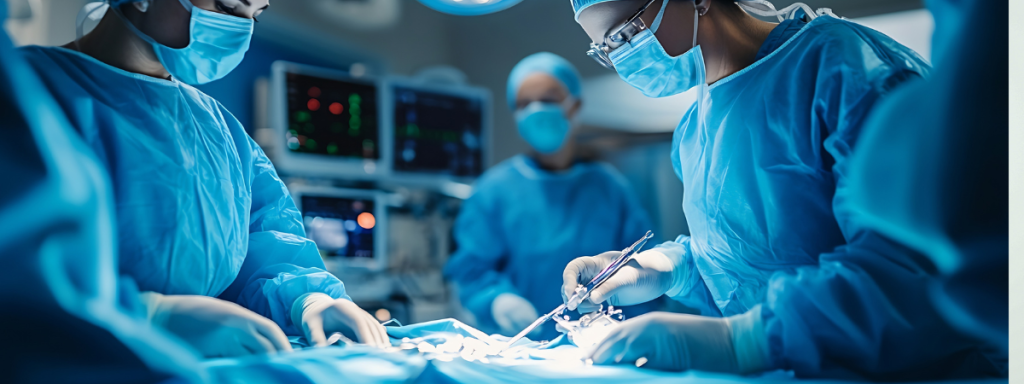
Read MoreWhich Spinal Surgeries Are Most Common After an Accident?
The spinal cord is responsible for communication with the brain and supporting you through all types of movement—so when a car accident, fall, or other accident leaves you in need of spinal surgery, it is normal to worry. There are several types of spinal surgeries that may be recommended after an injury, from discectomy and…
Read MoreHow to Maximize Your Settlement After a Truck Accident in Tennessee
Accidents with semis, tractor-trailers, and other large commercial trucks can cause serious injuries. Some injuries, such as traumatic brain injuries and spinal cord damage, may be life-changing. Many truck accident injuries are permanent, chronic, or require long-term medical care. Victims of truck accidents should be restored, as much as possible, to the financial, physical, and…
Read MoreTruck Driver Fatigue and Hours-of-Service Violations: Tennessee and Federal Rules Explained
Truck drivers and trucking companies understand the phrase, “time is money.” The more deliveries that a truck driver can make in a day or a week, the more money both the driver and the trucking company can earn. Many truck drivers push the limits of how many hours they drive in order to get back…
Read MoreCan You Recover Damages If You Were Partially at Fault in TN?
In most types of accidents in Tennessee, victims can recover damages even if they are partially responsible for the accident – provided their share of responsibility is less than 50 percent. The ability to recover partial damages applies to most types of accidents, including: Car, truck, motorcycle, Uber, Lyft, bus, and other types of vehicle…
Read More